Biodiversity & Environment
Climate Change and Rising Health Risks
This editorial is based on “Climate change as a public health emergency” which was published in The Hindu on 07/04/2026. The article brings into perspective the growing reality of climate change as a public health crisis, highlighting its role in intensifying diseases, heat stress, air pollution, and food insecurity in India.
For Prelims: Global Warming, Particulate Matter, National Programme on Climate Change and Human Health (NPCCHH).
For Mains: How climate change exacerbates health concerns, How India is Tackling challenges posed by Climate health nexus, what further measures are needed.
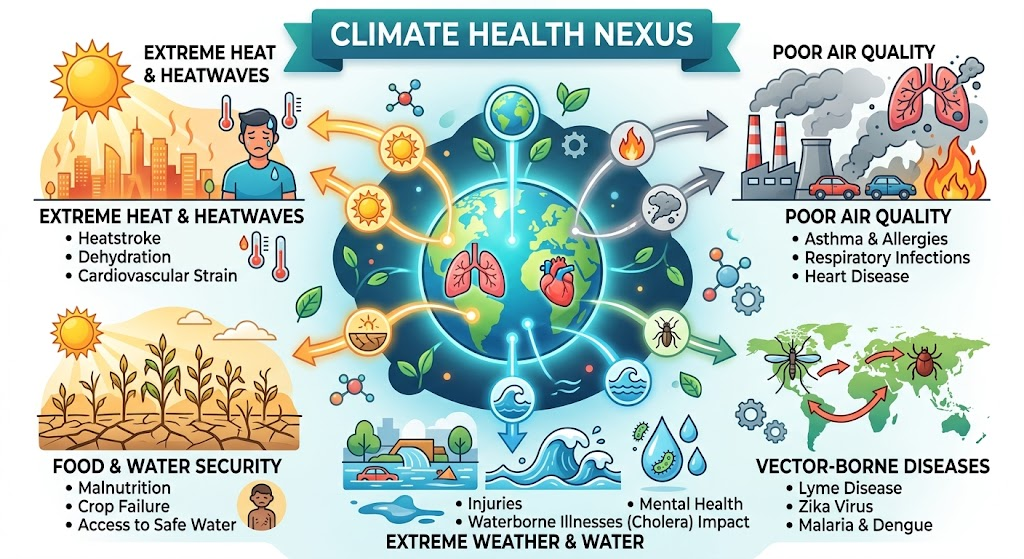
Climate change is no longer a distant environmental concern but an immediate public health emergency, with India witnessing rising heatstroke deaths in regions like Odisha and Telangana and shifting dengue peaks from September to November in Delhi-NCR. Expanding vector habitats and erratic rainfall are increasing the spread of diseases like malaria into previously unaffected regions such as Himachal Pradesh. Simultaneously, elevated PM2.5 levels and heat stress are aggravating cardiovascular, respiratory, and renal disorders, contributing to a growing non-communicable disease burden. Coupled with climate-induced food insecurity and malnutrition, these trends underline that climate change is fundamentally reshaping India’s health landscape.
How Climate Change Exacerbates Health Concerns?
- Extreme Heat and Occupational Mortality: Escalating baseline temperatures and prolonged heatwave durations critically overwhelm human thermoregulation, inducing fatal heatstroke and acute renal failure.
- This extreme thermal stress disproportionately imperils India's massive unorganized sector, particularly agricultural and construction laborers lacking adequate cooling respite.
- The Lancet Countdown report reveals that in 2024, Indians experienced a record 19.8 heatwave days in 2024, causing the loss of 247 billion potential labor hours.
- Vector-Borne Disease Expansion: Rising baseline temperatures, erratic monsoons, and shifting humidity regimes expand the geographical range and breeding longevity of Aedes and Anopheles mosquitoes across the subcontinent.
- This altered ecology significantly shortens the viral incubation period within vectors, accelerating explosive urban outbreaks and introducing diseases to previously non-endemic, high-altitude zones.
- Recent health ministry data highlights a massive surge in the nation's dengue burden, climbing to over 2.33 lakh by 2024.
- Furthermore, states like Tamil Nadu and Kerala are now reporting perennial transmission.
- Respiratory Pathologies from Air Pollution: Climate-driven meteorological stagnation, delayed monsoons, and intensified biomass burning create severe inversion layers over the Indo-Gangetic Plain, trapping toxic particulate matter.
- Prolonged exposure to these extreme pollution concentrations chemically inflames the respiratory tract, critically exacerbating asthma, chronic obstructive pulmonary disease (COPD), and pediatric lung underdevelopment.
- A Lancet report reveals human-caused PM2.5 pollution led to over 17 lakh deaths in India in 2022, a 38% rise since 2010.
- Waterborne Pathogens via Hydrological Extremes: The increasing frequency of climate-intensified cyclonic storms and erratic extreme precipitation events routinely overwhelm aging municipal drainage systems, contaminating potable water with raw sewage.
- This systemic breakdown of sanitation infrastructure creates an optimal ecological breeding ground for explosive, multi-state outbreaks of enteric infections and acute diarrheal diseases.
- Following catastrophic urban flooding events in states like Sikkim, Assam, and Kerala recently, local health authorities consistently documented massive surges in cholera and typhoid.
- National health profiles indicate these hydrological disasters disproportionately impact vulnerable demographics, with waterborne pathogens remaining a leading cause of preventable pediatric hospitalizations across flooded regions.
- Nutritional Deficiencies from Agricultural Degradation: Anthropogenic climate change physically disrupts India’s agrarian economy through prolonged heat stress and elevated atmospheric CO2, which paradoxically dilutes essential micronutrients in staple crops.
- This twin threat of diminished harvest volumes and degraded cereal nutritional quality drastically elevates the baseline risk of chronic malnutrition, anemia, and childhood stunting.
- Current models by the Indian Council of Agricultural Research (ICAR) project that unmitigated climate shifts will reduce rain-fed rice yields by 20% and wheat yields by 19.3% by 2050.
- Simultaneously, elevated CO2 levels are proven to reduce protein, zinc, and iron concentrations in staple grains, exacerbating India's existing hidden hunger crisis.
- Amplification of Zoonotic Epidemics: Progressive deforestation combined with erratic rainfall fundamentally alters the migratory and foraging behaviors of indigenous wildlife, driving them into densely populated peri-urban agricultural zones.
- This unprecedented ecological proximity collapses the species barrier, vastly increasing the spillover probability of highly virulent zoonotic viruses into immunologically naive human populations.
- The recurring, high-mortality Nipah virus outbreaks in Kerala, which resurfaced aggressively in recent years, are directly tied to climatic stress forcing fruit bats out of traditional forest habitats.
- Escalating Eco-Anxiety and Mental Health Crises: The psychological toll of climate change manifests as a profound mental health crisis in rural India, where agrarian livelihoods are entirely dependent on highly volatile climatic stability.
- Repeated catastrophic crop failures due to cyclical droughts, unseasonal hailstorms, and extreme heatwaves inflict acute chronic stress, paralyzing debt traps, and deep-seated eco-anxiety.
- Empirical socio-economic studies consistently link severe drought years in vulnerable agricultural belts like Vidarbha and Marathwada to tragic, localized spikes in farmer suicide rates.
- Furthermore, recent public health surveys note a sharply rising trend in clinical depression and post-traumatic stress among agricultural laborers, exacerbated by a near-total absence of psychiatric support infrastructure.
- Disruption of Healthcare Infrastructure: Extreme weather phenomena not only create secondary health crises but actively dismantle the physical and structural capacity of the healthcare system to respond to these emergencies.
- High-intensity cyclones and unprecedented urban flooding routinely submerge primary health centers, sever critical supply chains for life-saving therapeutics, and plunge hospitals into prolonged blackouts.
- During recent high-category cyclones on the Eastern coast and devastating 2025 floods in Northeastern states, dozens of rural health facilities were structurally compromised or rendered entirely inaccessible.
- This infrastructural paralysis fatally delays critical acute care interventions, leading to a sharp rise in preventable secondary mortalities long after the immediate meteorological disaster has dissipated.
What Measures Has India Adopted to Address the Climate Health Nexus?
- Institutional Governance via NPCCHH: The National Programme on Climate Change and Human Health (NPCCHH) establishes India's foundational governance architecture for mainstreaming climate adaptation directly into public health policy.
- This institutional framework shifts the healthcare paradigm from reactive disaster management to proactive surveillance, capacity building, and climate-sensitive disease mitigation.
- Implementation of Heat Action Plans (HAPs): To combat escalating extreme heat mortality, India has institutionalized localized Heat Action Plans (HAPs) that mandate inter-departmental coordination, occupational safeguards, and early warning dissemination.
- These multidimensional plans protect socioeconomically vulnerable demographics by enforcing shaded work-hours, establishing public cooling shelters, and ensuring hospital surge-capacity readiness.
- In collaboration with the National Disaster Management Authority (NDMA), robust HAPs were actively executed across 23 highly vulnerable, heat-prone states during the severe 2024 and 2025 summers.
- Daily heat-related illness tracking on the Integrated Health Information Platform (IHIP) successfully monitored tens of thousands of cases, utilizing granular data to optimize immediate medical deployments.
- Launch of the National One Health Mission: India has launched the National One Health Mission to comprehensively mitigate the rising threat of zoonotic disease spillovers driven by climate-induced ecological and habitat disruptions.
- By inherently integrating human, veterinary, and environmental health sectors, this holistic approach dismantles institutional silos to preemptively detect and contain novel pathogens before they trigger pandemics.
- Backed by a substantial ₹383 crore investment and the recent establishment of the National Institute of One Health in Nagpur, the mission formally centralizes cross-ministerial disease intelligence.
- Transition to Green Healthcare Infrastructure: Acknowledging the healthcare sector's own carbon footprint, India is aggressively pursuing the decarbonization and climate-proofing of medical infrastructure through distributed renewable energy integration.
- This transition to green hospitals ensures uninterrupted, life-saving critical care during extreme weather-induced grid failures while systematically reducing the sector's long-term operational greenhouse gas emissions.
- Under the updated NPCCHH guidelines, health facilities are increasingly adopting climate-resilient building standards and solarization, bridging climate adaptation with tangible mitigation.
- Deployment of Precision Early Warning Systems: The Indian Meteorological Department (IMD) has revolutionized its predictive capabilities by deploying Multi-Model Ensemble (MME) forecasting, directly linking advanced climatology with preemptive public health interventions.
- The India Meteorological Department follows a seamless multi-scale forecasting strategy, providing nowcasts up to six hours and short- to medium-range forecasts up to seven days across regions.
- This highly granular, impact-based meteorological data allows district administrations to execute targeted evacuations and preposition medical supplies well before extreme weather events strike.
- Air Pollution and Respiratory Health Action Plans: Addressing the lethal synergy between climate-induced atmospheric stagnation and particulate matter, India has integrated specialized Air Pollution and Health Action Plans within its broader climate strategy.
- This policy matrix focuses on chemically identifying inversion-trapped pollutants and preemptively managing the consequent surge in acute respiratory distress, asthma exacerbations, and cardiovascular emergencies.
- Concurrently, epidemiological surveillance networks are actively linking local Air Quality Index (AQI) telemetry with hospital emergency room admissions to dynamically allocate nebulizers and oxygen reserves.
- Real-Time Digital Epidemiological Surveillance: To counter the explosive spread of waterborne and vector-borne pathogens triggered by shifting monsoons and hydrological extremes, India has heavily digitized its epidemiological tracking infrastructure.
- Shifting from delayed, paper-based reporting to real-time digital dashboards allows epidemiologists to detect localized infectious disease clusters instantly and deploy rapid response teams effectively.
- The aggressive expansion of the Integrated Health Information Platform (IHIP) allows primary healthcare centers across all states to upload daily, verified incidence data on climate-sensitive diseases.
- Climate-Focused Psychiatric Resilience Protocols: Recognizing that environmental displacement and agrarian collapse inflict severe psychiatric trauma, India has proactively integrated psychological resilience into its climate-health nexus interventions.
- This essential integration addresses the rapidly rising tide of disaster-induced PTSD, eco-anxiety, and farmer depression by embedding specialized mental health protocols into post-disaster public health responses.
- Under the NPCCHH framework, the central government published dedicated Standard Operating Guidelines on Climate Change and Mental Health to train primary care physicians in disaster psychiatry.
What Further Measures are Needed to Counter Climate-Health Nexus?
- Micro-Climatic Vulnerability Mapping (Spatial Epidemiology): We must transition from macro-level climate models to hyper-local, geo-spatial health vulnerability mapping that cross-references micro-climatic anomalies with ward-level socio-economic demographics.
- This precision public health tool would enable municipal corporations to identify specific high-risk neighborhoods predisposed to extreme urban heat island effects or localized vector breeding.
- By overlaying epidemiological surveillance with real-time topographical and hydrological data, local governments can pre-emptively allocate targeted medical resources and targeted infrastructural upgrades.
- Such granular spatial epidemiology transforms passive hazard recognition into active, geographically precise preemptive health interventions.
- Integration of Climate-Resilient WASH Infrastructure: Addressing recurrent waterborne epidemics requires physically upgrading municipal Water, Sanitation, and Hygiene (WASH) infrastructure to withstand extreme hydrological volatility without systemic cross-contamination.
- Engineering interventions must mandate the implementation of decentralized wastewater treatment networks and flood-proof sanitation grids that physically separate stormwater runoff from critical sewage channels.
- Furthermore, incentivizing bio-filtration swales and permeable urban surfaces will naturally mitigate sudden deluge impacts, actively reducing the ecological breeding grounds for enteric pathogens.
- This structural climate-proofing ensures that baseline public hygiene remains fundamentally uncompromised even during catastrophic, high-intensity precipitation events.
- Climate-Adaptive Pharmacological Supply Chains: The medical sector must actively redesign its pharmacological supply chains to guarantee cold-chain resilience and therapeutic efficacy against extreme thermal and meteorological disruptions.
- Implementing decentralized, solar-powered medical refrigeration units at primary health centers will effectively insulate vital biologics, vaccines, and antivenoms from climate-induced regional power grid failures.
- Additionally, domestic pharmaceutical manufacturing needs to integrate predictive meteorological modeling to strategically stockpile emergency life-saving therapeutics well ahead of forecasted disaster seasons.
- Cross-Training Frontline Health Sentinels: To truly operationalize climate-health interventions at the grassroots level, we must actively cross-train our frontline community health workers in climate-syndromic surveillance and disaster first-response.
- Equipping grassroots personnel with specialized diagnostic protocols for heat exhaustion, early vector-borne symptoms, and waterborne pathogens accelerates immediate triage before institutional hospitalization becomes necessary.
- This localized capacity building empowers community workers to distribute oral rehydration salts, administer preliminary care, and disseminate targeted climate-health literacy directly to socioeconomically vulnerable households.
- Mainstreaming Eco-Psychiatry in Primary Healthcare: To combat the growing crisis of ecological grief and disaster trauma, public health frameworks must systematically integrate eco-psychiatry and trauma-informed care into routine primary medical services.
- Health ministries should formulate standardized screening protocols for post-disaster PTSD and chronic eco-anxiety, making psychological evaluations a mandatory component of post-calamity medical rehabilitation camps.
- By establishing decentralized, community-led psychosocial support groups facilitated by trained psychiatric nurses, governments can destigmatize mental health intervention among deeply impacted agrarian and displaced populations.
- This institutional mainstreaming of environmental mental health care builds long-term cognitive resilience, preventing acute distress from deteriorating into severe psychiatric morbidity.
- Agrarian Nutritional Diversification and Biofortification: Counteracting the climate-driven dilution of crop nutrients necessitates a strategic agricultural shift away from vulnerable monocultures toward the aggressive cultivation of biofortified, climate-resilient staple crops.
- Agricultural extension services must actively subsidize and distribute high-yield, drought-tolerant seed varieties like biofortified millets and iron-rich legumes that maintain their nutritional integrity under severe thermal stress.
- Synchronizing agricultural policy with public health nutritional programs ensures these fortified crops are directly integrated into public distribution systems and essential supplementary feeding schemes.
- This localized nutritional sovereignty structurally shields vulnerable pediatric and maternal demographics from the escalating threat of climate-induced hidden hunger and micronutrient deficiency.
- Dynamic Occupational Health Mandates for the Unorganized Sector: Protecting the massive informal workforce demands the formulation and strict enforcement of dynamic occupational health mandates that are directly triggered by real-time micro-climatic thresholds.
- Labor regulations must proactively evolve to mandate compulsory shaded rest periods, mandatory hydration intervals, and the shifting of peak physical labor to cooler diurnal windows during extreme heat alerts.
- Simultaneously, governments must innovate financial safety nets, such as micro-insurance models or climate-linked wage compensation, to reimburse daily wage earners for work hours lost to lethal weather conditions.
- This intersection of labor rights and climate adaptation prevents economically vulnerable populations from being forced to choose between severe financial destitution and fatal thermal exposure.
- Synthesizing Zoonotic Genomic Surveillance Networks: Preempting the next climate-induced pandemic requires the establishment of active, continuous genomic surveillance networks deeply embedded within high-risk ecological displacement zones and peri-urban agricultural borders.
- Veterinary and human public health authorities must collaboratively deploy mobile biosurveillance units to systematically sequence pathogens from livestock, displaced wildlife, and human populations concurrently.
- By utilizing advanced bioinformatics and machine learning algorithms to map unusual cross-species viral mutations in real-time, authorities can intercept localized zoonotic spillovers before they achieve exponential human-to-human transmission.
- This aggressive, proactive genomic monitoring transforms the collaborative health approach from a theoretical framework into a rapid-response, on-the-ground pandemic prevention shield.
Conclusion:
The climate-health nexus in India has evolved into a systemic crisis that demands a fundamental paradigm shift from reactive emergency management to proactive, climate-resilient healthcare governance. By integrating hyper-local vulnerability mapping with green infrastructure and community-led mental health support, India can bridge the gap between environmental policy and public well-being. Ultimately, a "Health-in-All-Policies" approach, rooted in the One Health philosophy, is essential to safeguarding the nation’s demographic dividend against the escalating volatility of a warming planet.
|
Drishti Mains Question "The intersection of climate change and public health in India is no longer an environmental prediction but a socio-economic reality." Critically analyze the multi-dimensional impacts of climate change on India’s health landscape. |
FAQs
1. What is the NPCCHH?
It is the National Programme on Climate Change and Human Health, aimed at building healthcare capacity to tackle climate-sensitive diseases.
2. How does climate change affect India's labor productivity?
Extreme heat leads to the loss of billions of labor hours (e.g., 247 billion in 2024), severely impacting the $194 billion informal economy.
3. What is the 'One Health' approach?
An integrated strategy that links human, animal, and environmental health to prevent zoonotic disease spillovers like Nipah.
4. How does CO2 affect nutrition in crops?
High atmospheric CO2 paradoxically reduces essential micronutrients like protein, zinc, and iron in staples like rice and wheat.
5. What are HAPs?
Heat Action Plans are localized strategic frameworks for early warning, cooling relief, and medical readiness during heatwaves.
UPSC Civil Services Examination Previous Year Question (PYQ)
Mains
Q. ‘Climate change’ is a global problem. How will India be affected by climate change? How Himalayan and coastal states of India are affected by climate change? (2017)
Q. “Besides being a moral imperative of a Welfare State, primary health structure is a necessary precondition for sustainable development.” Analyse. (2021)