Biodiversity & Environment
Zoonotic Diseases
- 01 Apr 2020
- 14 min read
Introduction
- The word 'Zoonosis' (Pleural: Zoonoses) was introduced by Rudolf Virchow in 1880 to include collectively the diseases shared in nature by man and animals.
- Later WHO in 1959 defined that Zoonoses are those diseases and infections which are naturally transmitted between vertebrate animals and man.
- Zoonoses may be bacterial, viral, or parasitic, or may involve unconventional agents.
- As well as being a public health problem, many of the major zoonotic diseases prevent the efficient production of food of animal origin and create obstacles to international trade in animal products.
How do germs spread between animals and people?
- Zoonotic transmission can occur in any context in which there is companionistic (pets), economic (farming, etc.), predatory (hunting, butchering or consuming wild game) or research contact with animals.
- Contamination of food or water supply: Eating or drinking contaminated food can cause various types of diseases in humans.
- Direct contact: While petting or touching animals, and bites or scratches.
- Indirect contact: Coming into contact with areas where animals live and roam.
- Vector-borne: Being bitten by a tick, or an insect, like a mosquito or a flea food-borne
Types of Influenza in Animals
- Most strains of influenza that infect humans are human diseases, although many strains of bird flu and swine flu are zoonoses.
- Influenza A viruses are found in many different animals, including ducks, chickens, pigs, whales, horses, seals, and cats.
- These viruses occasionally recombine with human strains of the flu and can cause pandemics.
- Bat influenza: Influenza A viruses are found in bats.
- Bat flu was first discovered in “little Yellow-shouldered bats” in Guatemala
- Internal genes of bat flu viruses are compatible with human flu viruses
- Influenza in cats: Cats can be infected with influenza viruses, including avian influenza viruses.
- Influenza in cats is thought to spread the same way that human flu spreads: through direct contact.
- Canine influenza (dog flu): A contagious respiratory disease in dogs caused by specific type A influenza viruses — H3N8, H3N2.
- No human infections with canine influenza have ever been reported.
- Swine/Variant influenza: A respiratory disease of pigs caused by type A influenza viruses.
- Avian influenza: These viruses occur naturally among wild aquatic birds worldwide and can infect domestic poultry and other bird and animal species.
- All subtypes of influenza A viruses apart from H17N10 and H18N11 can infect birds.
Classification of Zoonoses
According to the Etiological (Originating) Agents
- Bacterial zoonoses: e.g. anthrax, brucellosis, plague, leptospirosis, salmonellosis, lyme disease
- Viral zoonoses: e.g. rabies, arbovirus infections, KFD, yellow fever, influenza
- Rickettsial zoonoses: e.g. murine typhus, tick typhus, scrub typhus, Q-fever
- Protozoal zoonoses: e.g. toxoplasmosis, trypanosomiasis, leishmaniasis
- Helminthic zoonoses: e.g. echinococcosis (hydatid disease), taeniasis
- Fungal zoonose: s e.g. deep mycosis - histoplasmosis, cryptococcosis
- Ectoparasites: e.g. scabies, myiasis
According to the mode of transmission
- Direct zoonoses: Transmitted from an infected vertebrate host to a susceptible host (man) by direct contact, by contact with a fomite or by a mechanical vector. Eg: rabies, anthrax, brucellosis etc.
- Cyclozoonoses: Require more than one vertebrate host species, but no invertebrate host for the completion of the life cycle of the agent, e.g. echinococcosis, taeniasis.
- Metazoonoses: These are transmitted biologically by invertebrate vectors, in which the agent multiplies and/or develops and there is always an extrinsic incubation (prepatent) period before transmission to another vertebrate host e.g., plague.
- Saprozoonoses: These require a vertebrate host and a non-animal developmental site like soil, plant material, pigeon dropping etc. for the development of the infectious agent e.g. aspergillosis.
According to the reservoir host
- Anthropozoonoses Infections: Transmitted to man from lower vertebrate animals e.g. rabies, leptospirosis, plague, arboviral infections, brucellosis and Q-fever.
- Zooanthroponoses Infections: Transmitted from man to lower vertebrate animals e.g. streptococci, staphylococci, diphtheria, enterobacteriaceae, human tuberculosis in cattle and parrots.
- Amphixenoses Infections: Maintained in both man and lower vertebrate animals and transmitted in either direction e.g. salmonellosis, staphylococcosis.
Factors Influencing Prevalence of Zoonoses
- Ecological changes in man's environment
- Exploitation of new territories and natural resources like harnessing the power of rivers, constructing roads and pipelines through thinly populated areas, clearing, irrigating and cultivating new land, deforestation lead to entering of humans in the unaccustomed ecosystem in which potential pathogens form part of the biotic community (natural focus).
- Large scale expansion of agricultural and engineering resources, construction of dams, artificial lakes, irrigation schemes, clearing of forests -all these lead to changing of the biting habits of the blood sucking vectors and alteration in the population of reservoir animals which has led to the spread of such diseases.
- Handling animal by-products and wastes (occupational hazards)
- For eg- anthrax in carpet weavers, live stock raisers and workers with animal hair in the textile industry, leptospirosis in rice field workers, listeriosis in agricultural workers etc.
- Increased movements of man
- Land development, engineering project work, pilgrimages, tourism, etc. expose the people to contaminated food and water.
- Increased trade in animal products
- Wool, bone meal, meat, etc. from an area where some of the zoonoses are endemic, are likely to introduce the disease into new territories.
- Transportation of virus infected mosquitoes
- Eg- Aircraft, ship, train, motor and other vehicles bring the viruses in to a new area, e.g. yellow fever Chikungunya fever, dengue fever etc.
- Cultural anthropological norms
- For eg- in Kenya, people allow the dogs and hyenas to eat human dead bodies infected with hydatidosis. This helps to perpetuate the transmission cycle of the disease.
Case Studies
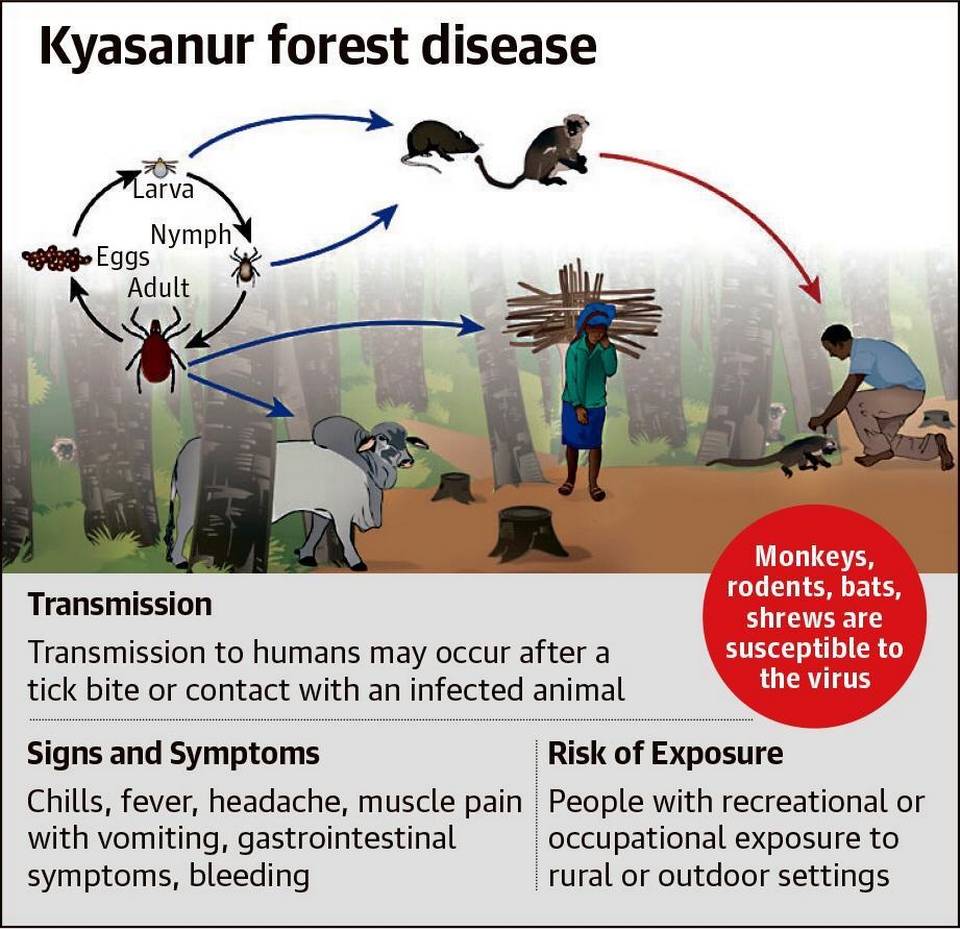
Kyasanur Forest Disease/Monkey Fever
- Kyasanur Forest disease (KFD) is caused by Kyasanur Forest disease virus (KFDV), a member of the virus family Flaviviridae.
- KFDV was identified in 1957 when it was isolated from a sick monkey from the Kyasanur Forest in Karnataka (formerly Mysore) State. Since then, between 400-500 humans cases per year have been reported.
- Hard ticks are the reservoir of the KFD virus and once infected, remain so for life.
- Rodents, shrews, and monkeys are common hosts for KFDV after being bitten by an infected tick.
- Another example of a zoonotic disease is COVID-19, which broke out in China's Wuhan district in December 2019.
- It was declared a pandemic by WHO in March 2020 with total cases reaching nearly 8 lakh.
- COVID-19 is caused by the virus SARS-CoV2 which is believed to have started in Huanan Seafood Wholesale Market in Wuhan.
SARS CoV
- Severe acute respiratory syndrome (SARS) emerged in 2002-2003 in southern China.
- SARS-CoV is thought to be an animal virus from an as-yet-uncertain animal reservoir, perhaps bats, that spread to other animals (civet cats) and first infected humans in the Guangdong province of southern China in 2002.
- An epidemic of SARS affected 26 countries and resulted in more than 8000 cases in 2003.
MERS CoV
- Middle-East respiratory syndrome (MERS) is a viral respiratory disease caused by a novel coronavirus (Middle East respiratory syndrome coronavirus, or MERS‐CoV) that was first identified in Saudi Arabia in 2012.
- Current scientific evidence suggests that dromedary camels are a major reservoir host for MERS-CoV and an animal source of MERS infection in humans.
Nipah
- The classic example of emergence of zoonotic disease is the outbreak of Nipah in Kerala.
- The virus can be transmitted to humans from animals (bats and pigs), and can also be transmitted directly from human-to-human.
- Fruit bats of the Pteropodidae family are the natural host of Nipah virus.
Zoonotic Diseases and India
- India is among the top geographical hotspots where zoonotics diseases are a major public health issue causing high burden of morbidity and mortality.
- High priority zoonotic diseases like Brucellosis have emerged from Haryana to Goa, incidence and prevalence of occupational zoonotic disease like Anthrax have affected human health throughout.
- Similarly, Bovine tuberculosis (bTB) is a chronic disease of cattle that impacts productivity and represents a major public health threat and is considered endemic in India.
- Further, being among the highest bacterial disease burden in the world, antibiotics, therefore, have a critical role in limiting morbidity and morality and consequently Antimicrobial Resistance (AMR) has huge implications for India.
- Major public health zoonotic diseases in India include Rabies, Brucellosis, Toxoplasmosis, Cysticercosis, Echinococcosis, Japanese Encephalitis (JE), Plague, Leptospirosis, Scrub typus, Nipah, Trypanosomiasis, Kyasanur forest disease (KFD) and Crimean-Congo haemorrhagic fever (CCHF).
- According to the National Centre for Disease Control (NCDC), about 75% of emerging and re-emerging infections are zoonotic, and new pathogens (viruses) continue to emerge and spread across countries.
Challenges to Controlling Zoonotic Diseases in India
- Large human population and its frequent interactions with animals.
- Poverty: Leads to increased dependence on animal rearing as a means of livelihood. The intimate human-animal contact puts them at risk for this category of diseases.
- Poverty-struck communities are primarily dependent on rearing animals as a means of livelihood and, therefore, the intimate human-animal contact puts them at risk for this category of diseases.
- Unawareness: Large part of population remains unaware of the basic hygiene routine to be followed.
- Lack of proper vaccination programmes, poor sero-surveillance and lack of diagnostic facilities make the preventive and precautionary approach more difficult.
Measures Taken ToControl Zoonotic Diseases
Following Programmes have been launched under National Centre for Disease Control:
- Integrated Disease Surveillance Programme (IDSP)
- National Programme for Containment of Anti-Microbial Resistance
- National Viral Hepatitis Surveillance Programme
- Strengthening Inter-sectoral coordination for prevention and control of Zoonotic Diseases of Public Health Importance
- National Rabies control programme
- Programme for prevention and control of Leptospirosis
Conclusion
- Zoonoses comprise a large percentage of all newly identified infectious diseases as well as existing infectious diseases.
- Cross-sectoral collaboration is key to understanding and managing public health risks at the human-animal-environment interface and improving global health security.
- Coordination between physicians, veterinarians, and epidemiologists should be strengthened.
- Technology should be used effectively. Each district and state in the country needs to be linked through satellite to the designated national headquarters for collecting real-time data on the activity of pathogens and diseases.
- International Organisations such as the WHO, Food and Agriculture Organization of the United Nations (FAO) and the World Organisation for Animal Health (OIE) should work in close collaboration to carry out expansive research in the field to prevent and manage the threats of such pandemics.
- The international community should also push for more transparency in the working of organisations such as WHO.