Governance
FFC Recommendations for Health Sector
- 19 Nov 2020
- 6 min read
Why in News
The Fifteenth Finance Commission (FFC) has made recommendations about the need for reprioritising public spending to fix the creaky health infrastructure exposed by the coronavirus pandemic.
- FFC has submitted its report to the President advising how to share tax revenues with states for the Financial Year (FY) 2022-26 period.
- The FFC report also makes recommendations about performance incentives to states in several reform areas.
Key Points
- Recommendations:
- FFC has mooted a greater role for public-private partnerships (PPPs) to ramp up the health infrastructure and scale up public spending on health from 0.95% of GDP to 2.5% by 2024.
- While public outlays should focus on primary health care at the panchayat and municipality level, private players should be relied on for specialty healthcare.
- The total spending of around 0.95% of GDP is not adequate in relation to the commitments under the National Health Policy of 2017.
- The 2017 Policy proposes raising public health expenditure to 2.5% of the GDP in a time-bound manner.
- There is a need for a more holistic approach to encouraging PPP in the health sector. There should be a constant working relationship and the government should not resort to the private sector in the case of an emergency only.
- The trust deficit that exists between industry and government needs to be bridged.
- District hospitals can become great grounds for training paramedics, creating health and employment multipliers.
- FFC Chairman emphasised on the need to create a cadre for medical officers as mentioned in the All India Services Act 1951.
- All-India health service is needed to address issues within the health sector.
- There is a need for substantial improvements in the working conditions for doctors in government hospitals, many of whom are hired on a contract basis by States.
- FFC has mooted a greater role for public-private partnerships (PPPs) to ramp up the health infrastructure and scale up public spending on health from 0.95% of GDP to 2.5% by 2024.
- Issues in the Health Sector:
- India’s general government expenditure on healthcare as a percent of GDP was just 1.0% in 2017, according to the World Health Organisation (WHO) data, placing it at number 165 out of 186 countries in terms of government expenditure on healthcare.
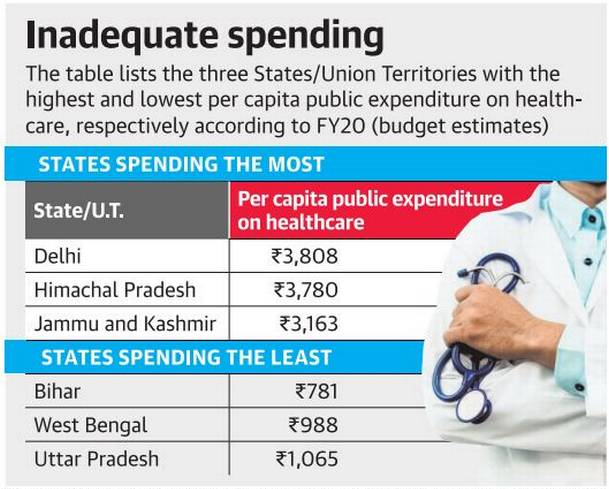
- Skewed availability of healthcare across India as poorer States have the worst facilities.
- In terms of access and quality of health services, India was ranked 145 out of 195 countries in a Lancet study published in 2018, below countries like China (48), Sri Lanka (71) Bhutan (134) and Bangladesh (132).
- Availability of trained epidemiologists is an issue due to low salary and job insecurity in the health system.
- There should be one epidemiologist per 0.2 million population. An epidemiologist is a technical person to guide and monitor the process of contact-tracing, marking containment zones and isolating suspected cases.
- India’s expenditure on R&D as a percent of GDP has continued to remain stagnant at 0.7% of GDP for three decades, with the public sector accounting for 51.8% of national R&D expenditure.
- This compares to around 2.8% of GDP for the USA, 2.1% of GDP for China, 4.4% of GDP for Korea and around 3% for Germany where the dominant sector by spending on R&D is the private sector.
Recent Initiatives
- Recently, the government has expanded the provision of financial support by means of viability gap funding for Public Private Partnerships (PPPs) in infrastructure projects to social sectors such as health, education, water and waste treatment.
- Several public-private partnerships and collaborations are already underway. The Defence Research and Development Organisation (DRDO) which has developed ventilators, collaborated with industry to scale up production of ventilators.
- There have been several examples of how public research laboratories, public institutions like the IITs, and private players including startups have risen to the challenge of working on Covid-19 testing kits, masks, alcohol-based sanitizers, personal protective equipment (PPEs) and ventilators, to overcome challenges of global supply chain disruptions and to cater to domestic needs.
- The government has made several interventions in the health sector including National Medical Commission, National Digital Health Mission, Ayushman Bharat, etc.
- A total of 17 Global Health Security Agenda (GHSA) projects have been started in India, with different government and private organisations.
- GHSA, set in 2014, builds on the WHO International Health Regulations (IHR) that provide guidance for countries to assess and manage serious health threats that have the potential to spread beyond borders.
- Capacity-building of the healthcare workers for surveillance and outbreak investigation is a vital step under workforce development of GHSA’s action package.
- One of the institutes responsible for workforce development under GHSA is the National Institute of Health and Family Welfare (NIHFW), that has implemented the “Public Health Systems Capacity Building in India” project.